News
“Fund Us Like You Want Us To Win”
"Fund Us Like You Want Us to Win” | The 68th Commission on the Status of Women (CSW68) By Alvin Massy,
UNGA Week Highlights From the perspective of Sybil Henry, Manager, Partnerships
2023 UNGA Week Highlights UNGA Week Highlights: From the perspective of Sybil Henry, Manager, Partnerships Bridging the Gap between Philanthropy & Nonprofits: Beyond MacKenzie Scott’s
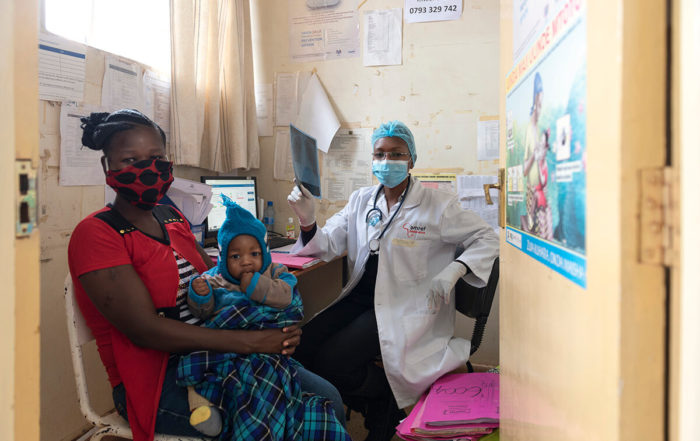
Press Release: Building a Fit-For-Purpose Health Workforce for Africa
News HISTORIC $100M CLINTON GLOBAL INITIATIVE COMMITMENT TO STRENGTHEN AFRICAN HEALTH WORKFORCE WITH AMREF HEALTH AFRICA & SEED GLOBAL HEALTH Strategy will support scaling
Roe v. Wade and What it Means to Us
At Amref Health Africa, we see first-hand the devastating effects illegal abortion has in the countries we work in. Unsafe abortion is a leading cause of
Amref’s COVID-19 Response
Amref is the leading Africa-based healthcare NGO on the frontlines of Africa’s COVID-19 response. Through the support and collaboration of our many partners, Amref is implementing a